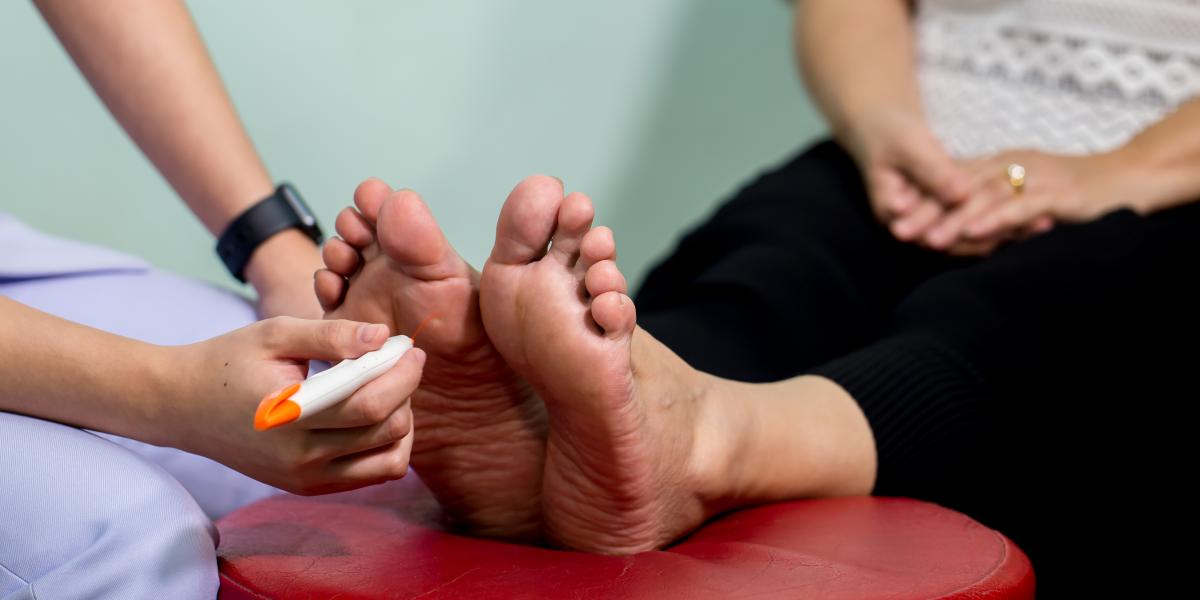
Neuropathy is damage to the nerves; it can occur in people who have diabetes. Then it is called diabetic neuropathy. Diabetes is a condition involving high levels in the body of blood sugar, or glucose. These high levels may injure nerves anywhere in the body, but most frequently they target the nerves in the diabetic’s feet and legs. The affected nerves have differing symptoms. Diabetic neuropathy can result in feelings of pain or numbness in the diabetic’s feet and legs. It can also lead to difficulties with the digestive system, blood vessels, urinary tract, and heart. While some diabetics experience mild symptoms of neuropathy, others find it extremely painful and even disabling. As many as half of all diabetics may suffer the complication to their condition that is diabetic neuropathy. However, diabetics can prevent or slow the appearance of and progress of neuropathy with consistent management of blood sugar along with a healthy lifestyle.
How Does Diabetic Neuropathy Come About?
People with difficult to manage diabetes, have had its management neglected, or have had it for a longer time than newer patients are more likely to experience the damage to their nerves of diabetic neuropathy. Neuropathy occurs when a high level of sugar or fats in the diabetic’s blood cause damage to nerves. Because nerves are a message service running throughout the body, this damage can cause a wide array of symptoms. Nerves are, in fact, essential to the working of the body. They allow people’s senses to report input to the brain, permit people to move, and control such functions that are automatic, like breathing. Diabetic neuropathy can come about in four different types:
- Mononeuropathies, which impact an individual nerve.
- Proximal neuropathy, damaging nerves along particular distributions in a diabetic’s body, such as in the legs or chest wall.
- Autonomic neuropathy, occurring in those nerves that control digestion or heart rate.
- Peripheral symmetric neuropathy, impacting the hands and feet. (This is the most common)
Signs and Symptoms
Symptoms of diabetic neuropathy may take years to appear. Particular signs and symptoms are linked to the different kinds of neuropathy. Peripheral neuropathy includes sensations that begin in the fingers and toes, continuing up arms or legs. These feelings include pain, numbness, burning, and tingling. The feet and hands may lose muscle tone or have difficulty feeling cold, heat, or injury. A loss of balance may result from peripheral neuropathy, as can joints breaking down in the feet, known as Charcot’s joint. Autonomic neuropathy has a much wider range of symptoms because it affects more than the hands and feet. Signs range from heartburn to faster heart rate, the inability to feel low sugar level effects to muscle weakness and contractions, and bladder problems to excessive sweating. Proximal neuropathy tends to cause pain in one side of the lower body with leg weakness. Focal neuropathy can impact the eyes and lead to visual disturbances like double vision.
Treatment and Prevention
Most varieties of diabetic neuropathy worsen as time progresses. Treatment for any type begins with bringing blood sugars into a doctor’s recommended target range. Management of high blood pressure, in addition to levels of cholesterol, goes hand in hand with this blood sugar control. Managing the levels of one’s glucose minimizes one’s chances of developing diabetic neuropathy. Generally, one key aspect of treatment is based on a focus on pain reduction and symptom management. Certain physical therapy types and medications can ease diabetic neuropathy’s pains. The nerves, however, are not repaired. Treatment also advises against smoking or excessive drinking of alcohol. Women should limit themselves to a single drink a day, while men have a limit of two drinks.